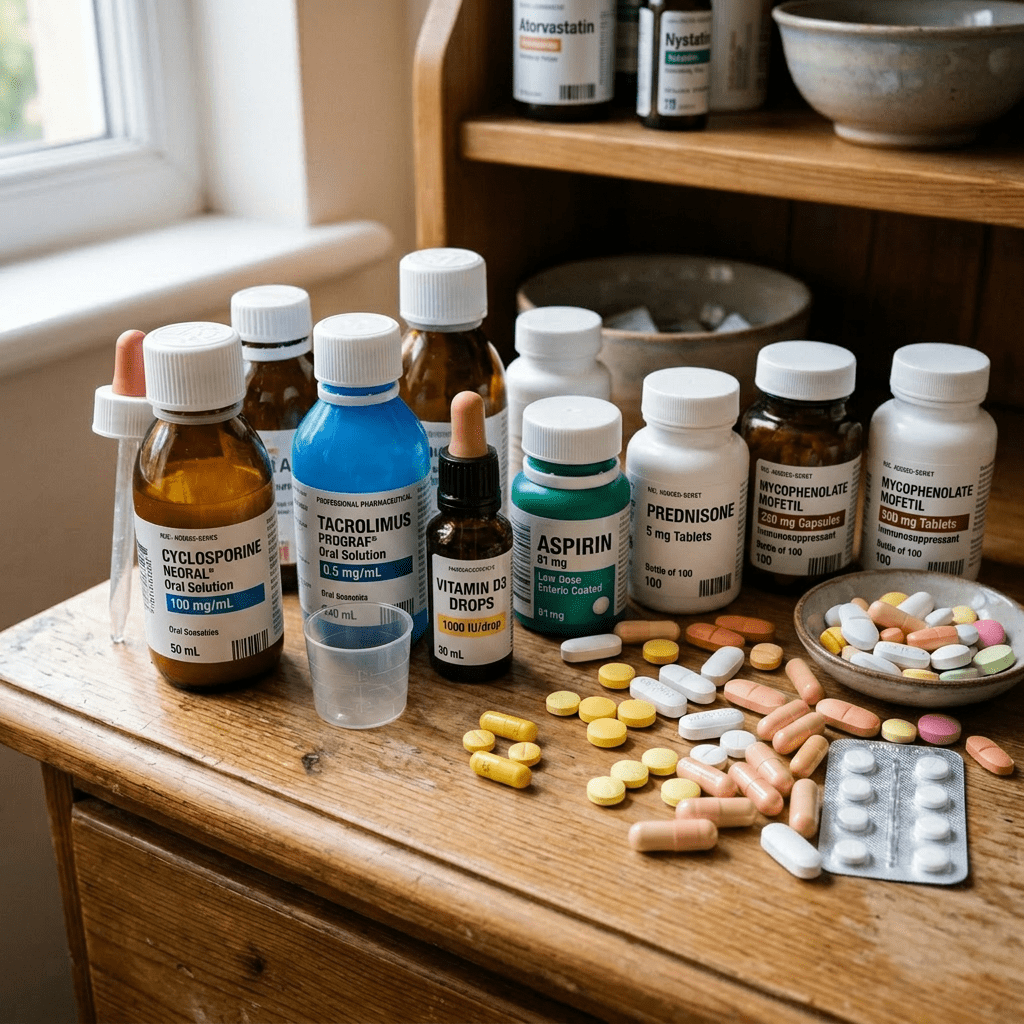
Medication Concepts
A good friend of mine who was also a heart transplant recipient once told me, “A heart transplant is not cure. It is more like a science project that never ends.” The daily discipline of taking medications is a big part of this science project’s success.
I will break this subject into 2 separate posts. This is the first topic which is a review of what my wife and I would consider important concepts. These thoughts are a collection of what we have learned over the past 2 years since the operation. I am not preaching, nor am I proposing that what is written here is the only view on this aspect. This is how we view this topic.
Simply stated, we feel the patient and the caregiver should know every aspect of each medication involved. This seems like it would be obvious; however, it is not easy when there are numerous unfamiliar meds, and the patient has just gone through a physical and mental trauma.
The medical center where I had my transplant placed a strong emphasis on education regarding medications among several other important topics. Most of this education takes place right after the transplant and is required before discharge. I was not 100% mentally sharp. Less even than usual. I was fuzzy from lack of sleep. I was still recovering from a surgical ordeal and large amounts of all kinds of drugs coursing through my veins related to anesthesia, pain management and meds you will read about here.
With regards to the medications I was taking specifically, in no uncertain terms the medical staff followed a very consistent and steady methodology that goes something like this:
- They told me what they are going to teach me and explained the importance of managing the medications properly.
- They taught me. Nearly every time I was given a medication, they showed it to me and told me the name, the dosage and it’s purpose.
- They asked me to tell them what they taught me. As I got closer to discharge, they would hold up a pill, or liquid and ask me what it’s name is, when I take it, what the dose is and why I was taking it.
- They told me to show them what they taught me and literally had Lauren and I fill up my medication pill box right before discharge. OK, Lauren did this.
- They gave us documentation of what they taught in writing. One of the many sections in a three-ring binder.
DYNAMIC, NOT STATIC
The medications after transplant change sometimes weekly, monthly, quarterly or randomly with medications changing doses, new medications starting and some medications stopping as recovery moves along.
Again, this is all happening when the patient is very banged up, and sort of foggy. These meds are coming at 7 am, 9 am, 1 pm, 6:30 pm and 9 pm. About a dozen different drugs. Probably 40 pills. In addition to pills, some meds are oral liquids. Some are injected. It’s a lot.
Over time, as my head cleared, I came to understand the importance of the knowing all of the aspects of each medication. I would say this is true for everyone who takes any kind of medication, even if it’s only one.
Know The Names of Each Medication and How to Pronounce Them
Most of these medications go by several names. There are the generic names and the brand names. For example, one medication I take to prevent organ rejection carries the name Tacrolimus. This is the generic name. The brand name is Prograf. I will take this medication for the rest of my life, unless it is substituted for a different organ rejection prevention medication. If I stop taking it, my body will eventually reject the implanted heart. Another more common example on naming is Levothyroxine. I take this for my thyroid unrelated to the heart transplant. Levothyroxine is a generic name whose brand name is Synthroid (among others). Know the names. Practice pronouncing them. Another good example of a hard to pronounce drug is Valgancylovir {val gan cyclo veer}. We keep a spreadsheet listing both the generic and brand names.
Be Able To Identify Each Medication By Sight
I was tasked to identify each medication I take by looking at it. A lot of these meds look alike. Pills have distinguishing features that set them apart. The shape, the size, the color, and maybe some kind of characters imprinted on the pill make them identifiable.
This can be tricky at times. As an example, Mycophenolate {my ko phen a late} looks very similar to Valgancyclovir (an anti-viral drug to prevent CMV / cytomegalovirus infections). At my doses both are large, oval, maroon-colored pills that are hard to tell part. The color shading and the exact oval shapes are slightly different.
Why is recognizing the meds by sight important? Let’s say it’s been a year since my transplant, and I am going to play golf. My tee time is 9:30 am. I am in my car at 9 am and decide wisely to take my 9 am meds now. I empty my 9 am meds from my pill box into my hand and clumsily spill some of the pills in, on or around the front seat of my car. I proceed to look everywhere and can successfully find 8 of the 11 pills I am supposed to take. Wouldn’t it be nice to know which ones I have found, and which are missing? This happened to me. Over the last 800 days (2,400+ times I’ve taken meds) since my operation, something similar has happened more than once.
Know Your Dose for Each Medication
Doses will change with frequency on many of these medications. We track this by noting it on our spreadsheet. When a dose changes we not only change the dose on our spreadsheet but make a notation at the bottom noting the date and the change.
Along with this we track the number of pills that make up the dose. I take a 1500 mg dose of Mycophenolate at 9 am and 9 pm every day. That dose is made up of 3 pills each containing 500 mg (and looks a lot like Valganciclovir). Are you getting the picture? I also take 20 mg of Torsemide every morning to remove excess fluid. I happen to have a large supply of 10 mg Torsemide pills because my dose has changed. So, I take 2 of the 10 mg pills to make up the 20 mg dose. On the spreadsheet we have one column as the dose. The next column is the number of pills. Keep in mind some of these meds will be taken more than once per day at very specific times.
Know the Purpose of Each Medication
The way it was explained to me is that each medication serves a general purpose and a has a specific role in maintaining my health. In the transplant world it breaks down into 3 main categories of purpose.
- Anti-Rejection Meds (i.e. Tacrolimus, Sirolimus, Mycophenolate, Prednisone)
- Anti-Infection Meds (including anti-viral, anti-bacterial and anti-fungal)
- Meds and Supplements Needed Because of the Meds in A & B (as an example, taking Prednisone on a long-term basis can negatively affect bone density so a calcium supplement may be prescribed).
Personal Other: I take a thyroid medication I mentioned unrelated to my heart issues. I have for decades. Another example is Ambien / Zolpidem which I take as needed for sleep. We add those to the spreadsheet.
Knowing the purpose of each medication is important so that there is a clear understanding of why. A patient may want to question their doctor if it is needed or how long they need to take it.
One of anti-fungal meds I took right after transplant was a nasty tasting liquid that I took three times a day. I was directed to swish it around my mouth first, then swallow and not eat or drink anything afterward for 30 minutes. It’s called Nystatin. I asked the nurse why I was taking it. What fungus was it preventing? She told me it prevents thrush. I asked her what thrush was. She said it’s like getting athletes foot all over the inside of your mouth. Once I heard that, I did not mind taking it so much. And I did not want to miss any doses of that. Why would I be vulnerable to getting thrush? Because anti-rejection meds lower the body’s natural immune system. Thankfully I was told I didn’t need to take it anymore 3 months post-transplant.
Know When During the Day You Take a Medication
I take meds at 7 am, 9 am, 1 pm, 6:30 pm and 9 pm. I won’t list each medication I take in each of those time slots, but suffice it to say, this takes close management. Some meds I take once per day. Some are twice during the day. We use a system where I AND my caregiver are assured I don’t miss any doses. Lauren and I both set alarms on our watches, and I try very hard to only hit STOP on the alarm after I have taken the meds for that time slot. I am notorious for hitting STOP with the intention of taking the meds, then some shiny object distracts my attention and then I miss all the meds in that time slot.

If I cannot take the meds at that time, then I hit the SNOOZE button on my watch alarm. If you don’t have a watch with an alarm, a phone will serve the same purpose. I really try to make sure I never miss a dose or a time slot for taking meds. I still fail. More often than I care to admit. Even with all those alarms. Remember, if I miss my 1 pm meds (for example), I will miss three different medications that should have been taken at that time slot. I have improved over time. Even after all these months it takes constant vigilance.
Some medications are lifetime. Some are temporary. After my transplant I was temporarily diabetic. I had never had diabetes before the transplant. Now, after two years I can stop taking any medication for my blood sugar level. My point is, regardless of the drug, I try to know what the parameters are for taking it. When can I stop taking it? I’ve always felt it a good thing when the doctor told me I can stop taking a certain medication.
CONCLUSIONS
Here are some reasons for all this attention to detail:
- As a patient I am asked constantly to review my medication list in detail. Every appointment that I attend with every doctor and every clinic (meeting with my transplant coordinator), and every procedure starts with a review of current medications. Same holds true with my meetings with my Primary Care Physician (PCP), dentist, and eye doctor. I bring my list to these events to make it easier.
- When I have all of this detail written or in spreadsheet form it makes filling the weekly pill box much easier.
- It helps Lauren and I understand which meds need refills, new prescriptions, and how much of each we have in reserve.
- I track the cost of each on my spreadsheet, which I admit is a little over the top. I want to know if I have a particular medication that costs an unusually high amount so I can look into how I might be able to lower that.
- I want to do the best that I can to follow the guidelines to be a great steward for the heart that was entrusted to me.
This will be continued to the next post, where I will explain how we have managed other aspects of medications as recovery progresses.
Leave a comment