By Phil Liaboe
Early Recovery
A major, historic nor’easter was forecasted to hit Boston on February 12th and 13th of 2024 but at the last minute it veered south and almost completely missed. The only weather that hit the city was a misty rain and some flurries. The city was shut down and a wide swath of surrounding towns had school closures in anticipation of the storm that didn’t happen. One of the earliest things I recall was looking out my 6th floor window of the Klarman building and seeing gray gloomy skies and glossy empty streets with the occasional Boston Police cruiser rolling by down below.
Keep in mind as you read, this is what happened to me. Every operation like this is unique and experiences can be very different, patient to patient.
I had no prior experience with waking up after prolonged general anesthesia. It was a tremendous strain to recall any of the names of the loved ones that were in the room with me. The first thing I recalled after I regained consciousness was my wife’s soothing and loving voice calling my name. I struggled to croak out hers. My concerned, wonderful daughters were there too.
My brain was a hazy fog and my surroundings were disorienting. I was heavily sedated and and in every way banged up. Amazingly I do not recall any pain with one very vivid exception. At some point I sneezed. That hurt a lot. Bright and sudden.
I later suggested to the kind social worker that the thick 3-ring information binder given to transplants candidates when they are added to the transplant list should have the words “DO NOT SNEEZE” on the cover. Anytime I had the slightest tickle or indication that a sneeze was imminent I would jam my finger up where my top lip joins the base of my nose and press. That works. Does it kill brain cells? Probably.
THIRSTY
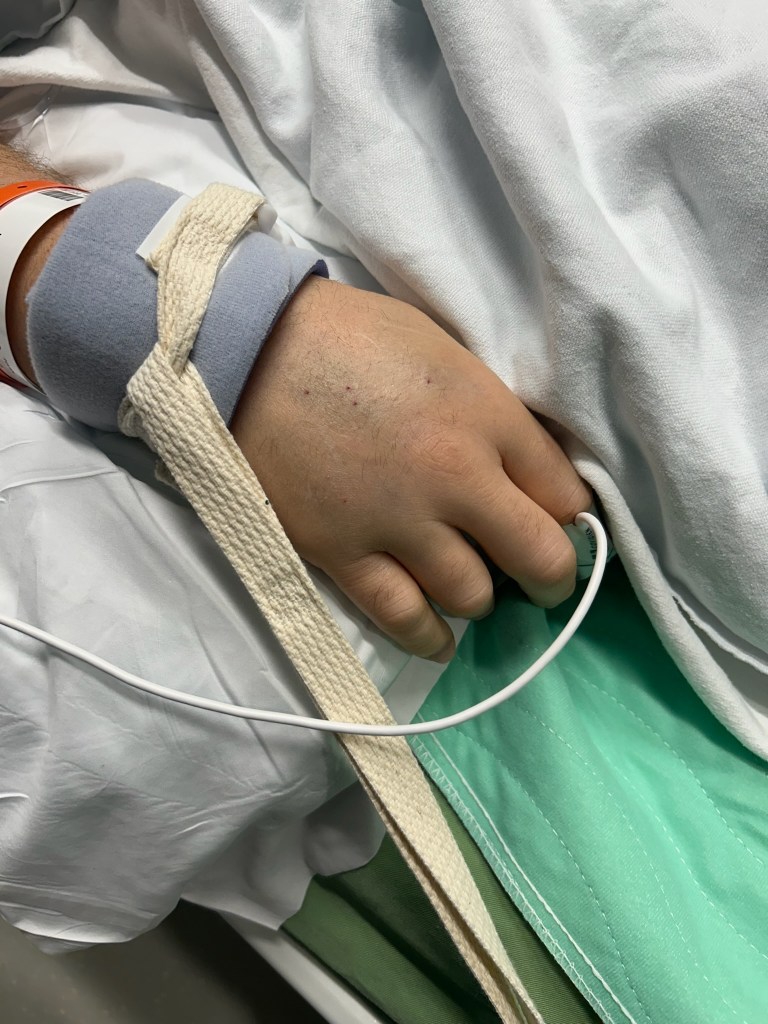
I do remember extreme thirst when I first woke up and early in my stay in the ICU. I would ask for water and the nurse would bring over a small styrofoam cup with a bent kiddie straw and put the straw to my dry cracked lips. Except she would keep her finger and thumb close to the straw and just when I got the tiniest bit of water, she clamped the straw so I could not get any more. That was annoying. I assumed there was a medical reason why I was not allowed to fill my mouth completely with cool fresh water like I wanted so badly.
COUGHING
I was coughing up a lot of phlegm. Enormous and mouth filling. It was frothy and snow white. I was told to spit it out and not to swallow that stuff in the early going. I began spitting it out into tissues. They gave me a small box of Kleenex, about the size of one of those travel size plastic wrapped packets, except in a box. I was going through those at a rate that the nurses could not replenish fast enough.
All this coughing up phlegm, I was told was due to being intubated and having an abnormal amount of fluid in my body. I could see that my hands were puffy beyond recognition and there was so much fluid it was leaking out of my eyes. Just clear fluid.
HEART SHAPPED PILLOW
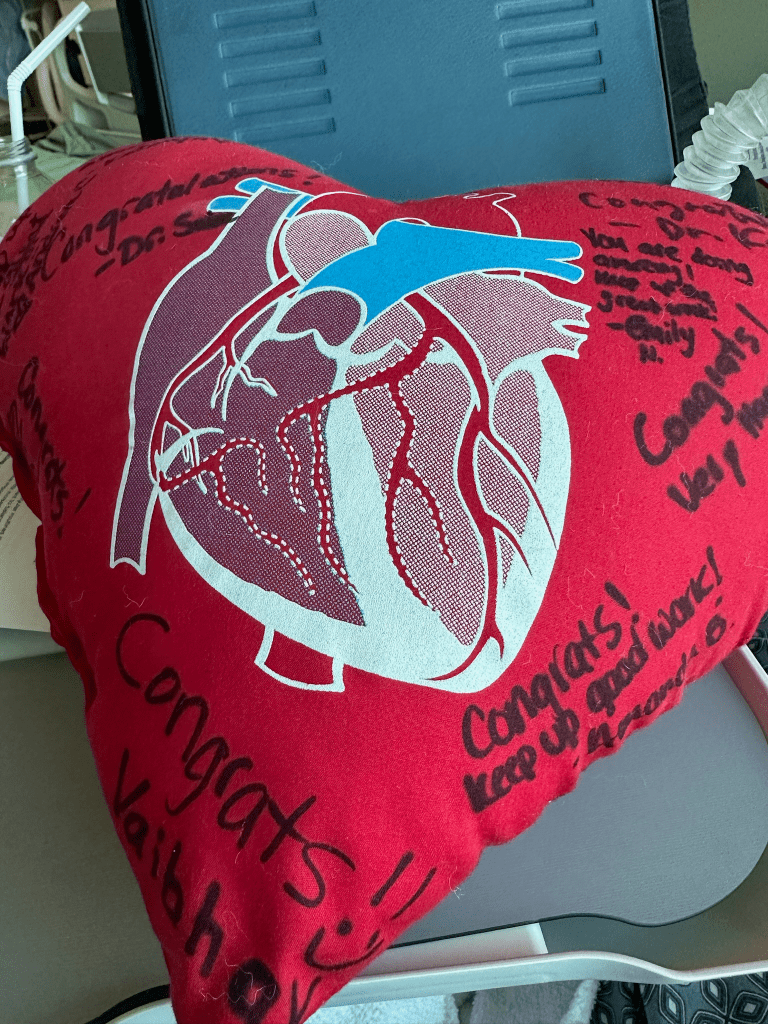
While in the Intensive Care Unit (ICU), one of the nurses caring for me handed me a heart shaped pillow and told me this was my new best friend. This freaked me out a little after considering the previous post.
The purpose of the pillow is for the patient to hold it tight to their chest when they cough. This is to reduce the stress on the sternum incision and keep the newly rejoined chest wall healing correctly. I carried it everywhere for several weeks. I used it many times each day. She was right! It was for that period, my new best friend.
INCISIONS
It was very unclear to me at that time exactly what was beneath the sheets that covered me. I knew there were bandages and wound dressings of all kinds. I did not at that point realize all that had been done to me surgically. I didn’t want to look.
I did not know what chest tubes were or that I had them. I did not know their purpose until I began writing this. I did not know when I woke up what ECMO was. Or that it was used on me and that I had more incisions to accommodate it.
SURROUNDINGS
To the right of my bed in the ICU was a battery of monitors, pumps, drips and IV bags. I think Lauren said there were about twelve, some with bags of fluid being administered. A catheter was draining my urine to a container next to my bad. Chest tubes were draining blood and fluid to another container next to my bed on the other side. I could not see those fluid containers nor did I know they existed.
WEAKNESS
I was very weak. For a day or two I could barely pull a Kleenex out of a Kleenex box. I was unable to operate my cell phone. I could pick it up. Touching one single correct button seemed as far away as playing golf.
NO HANDS OR ARMS ALLOWED
As I began my recovery my education regarding the best way to manage my new reality commenced. The most difficult physical short-term change I had to make was to maneuver in bed without using my hands or my arms. When I say short term, I mean about a month. This change is needed for the sternum incision to heal properly. This was in the forefront of my mind all the time.
I challenge anyone reading this to attempt it. Go ahead and lay down under the covers. Now roll over on your side. Now roll over on your other side. From that position, sit up to take a drink. Now, get out of bed to use the bathroom. Get out of a chair. Get up from a toilet. Do all these things without using your arms, or hands in any way. For a month.
Did the incisions hurt? My answer would be that they were sore enough to remind me they had been opened, but not enough to ask for more pain meds. I felt it the most during my coughing, trying to huck up the gunk the was persistently wanting to come out. These were not hard violent coughs. Every few minutes I felt a heavy rattle in my windpipe and one good exhale or gentle cough brought it up. I learned to cough gently.
For several days I had lidocaine patches on my chest that I assumed was for the pain of all my incisions. The nurses would regularly ask me about my pain level on a scale of 1 to 10 and I usually said it was a 2 or a 3. I don’t recall even asking for Tylenol. I might have.
ASH WEDNSDAY / VALENTINES DAY
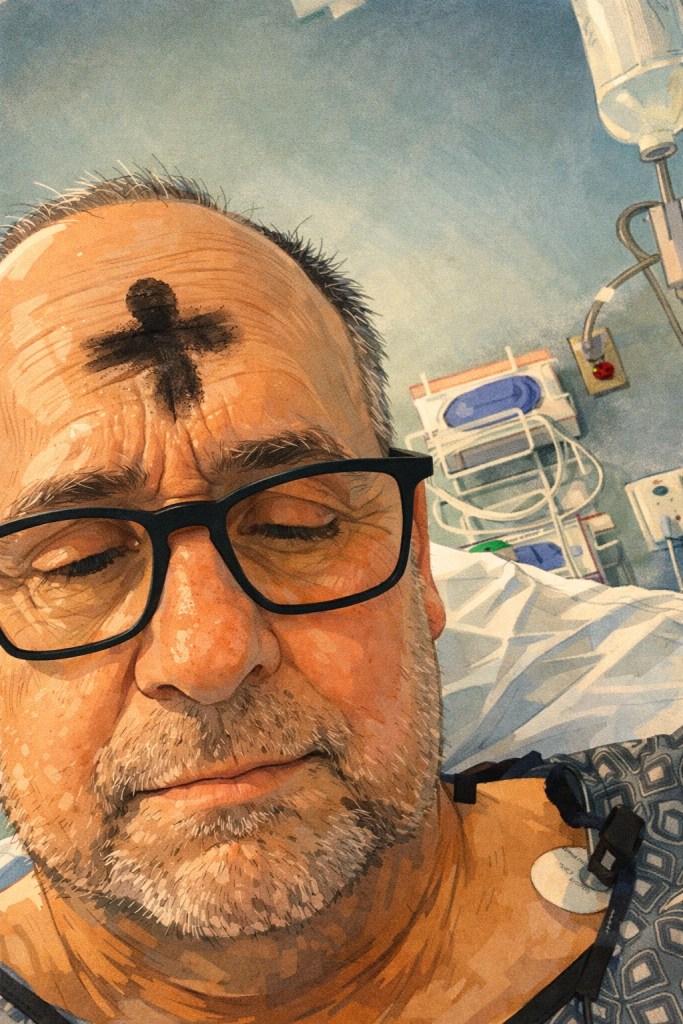
Another early awakening memory was that early in my coming around period it was Valentine’s Day & Ash Wednesday. Both on the same day. Valentine’s Day seemed like a little dash of kismet. That big red heart shaped symbol was everywhere right about the time I am starting to realize what it’s like to have a new heart. Not to mention that I had a heart shaped pillow that was now my new best friend.
Ash Wednesday is a day on the Christian calendar that signifies the start of the Lenten season. Lent is a forty-day period of reflection and spiritual reset acknowledging our sinful human nature and focusing on mortality, repentance and humility. It leads up to the recognition of the crucifixion and resurrection of Jesus Christ. Those who attend Ash Wednesday services will usually have a priest or pastor give the imposition of ashes on the worshiper’s forehead while the following words are spoken: “Remember that you are dust, and to dust you shall return”.
During that day a different Chaplin stopped by my room and asked if I wanted the imposition of ashes. I said that I did. I was sobbing as she made the cross of ashes on my expansive forehead.
EMOTIONS
Some of the side effects for me of the medications I was on and of surgery recovery were a very pronounced and overwhelming feeling of emotions coupled with and almost total inability to sleep.
On the emotional side, I was crying like a little girl at seemingly random times. I tried hard not to be weeping when the nurses were in the room. Sometimes I was upset thinking about the donor who had died and what their family must be going through. Sometimes it was tears of gratitude and euphoria and how very fortunate I was to get this kind of operation. Or I would think about the love from my family and all those helping me. Almost anything would set me off. It was a little embarrassing.
At about two years post-transplant some that is still with me.
FIRST STEPS

After only a day or two of regaining my senses the physical therapy people came in and said it was time to get up and walk. “Really?” I thought. There were three of them. The idea was that these therapists were going to instruct me on how to get myself out of bed. They would be there helping me while I used support to negotiate moving from my bed to the door of the room. Maybe fifteen feet.
I managed to get myself into a sitting position on the side of the bed without using my hands or arms. I got my feet on the floor and proceeded to stand up and when I did, I coughed a bit. That cough was hard enough to open the healing hole in my groin where the ECMO hose had been inserted. That’s a big blood vessel. Blood began running down my leg. Quite a lot of blood. It was a Dexter situation. There was enough blood splatter that the nice white HOKA sneakers worn by one of the nurses were a casualty.
Very quickly they sat me back down. A male nurse who had been taking care of me in the ICU came running with a big wad of dressing and slammed it into my groin to stop the flow. He held it there a long time. I offered to pay for the nurse’s sneakers that now had my blood on them. She would not hear of it. It all gets very real when you watch someone trying to clean your blood up off the floor with paper towels.
Later, we tried again. This time it went better. My puffy Michelin Man hands tightly gripped the handles on the back of an empty wheelchair for support. A white thick canvass belt was wrapped around my waist and a physical therapist held that belt behind me. A fall would be catastrophic. I am 6 feet 3 inches and at the time weighed 245 pounds. I made little baby steps to the door of my room and back in 20 minutes. It was a herculean task. It took all the strength and concentration I could muster. I was drenched in perspiration.
FAMILY AND FRIENDS
I was overwhelmed with support from my friends and family. I felt each and every one of their prayers. A very close friend of mine had coincidently had serious reconstruction surgery on his foot the same day of my operation. We commiserated about our current life changes, love for our families and for each other. Good friends and others I had not spoken to in many years reached out. It meant more than words can say. Lauren was by my side at every step, as were my daughters, living in the hotel across the street.
PEACE

A very welcome sensation that dawned on me very early on was one of absence.
The pounding that was in my chest was gone. For so long my native heart had been hammering away. Like it wanted out. And now it was quiet in there. No PVCs either. That fluttering that had been with me like a stink for several years was gone too. It hardly seemed real. No assisted devices. Just the new used heart doing it’s dance with a precision that I could not feel. For the first time I wondered what was keeping it pumping. I still don’t really know. I’ve read about it, but I could not explain it to anyone if I tried.
The next post will be my description of the Right Heart Catheterization / Heart Biopsy. This procedure features prominently in the recovery. Most patients will get 10 or 12 after tranplant. I’ve had more.
© 2026 Phil Liaboe. All rights reserved.
Leave a comment